As states implement reforms to address issues related to overuse and misuse of opioids, a new study released today by the Workers Compensation Research Institute (WCRI) observed decreases in the frequency and amount of opioids dispensed to injured workers in a majority of study states. However, higher utilization of opioids and other high-risk utilization patterns were seen in some states in the most recent study period.
“This report serves as a tool to monitor ongoing policy changes on opioid utilization in 26 state workers’ compensation systems. By comparing variations in the use of opioids across the states, this study can help policymakers and stakeholders be better informed about the level of opioid use in their states and better target future efforts to address issues related to prescription opioids in their states,” said Ramona Tanabe, WCRI’s executive vice president and in-house counsel.
The study, Interstate Variations in Use of Opioids, 4th Edition, examines interstate variations and trends in the use of opioids and prescribing patterns of pain medications across 26 state workers’ compensation systems covering data from October 2009 through March 2015.
The following are sample findings from the study:
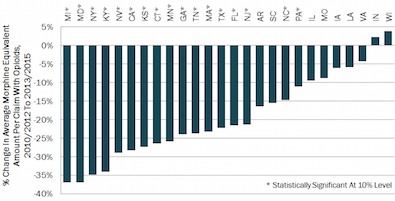
* Comparing opioid utilization for workers injured in 2010 and 2013 over an average two-year period following the injury, the study found reductions in the average amount of opioids dispensed to injured workers in several states, with larger reductions seen in Kentucky, Maryland, Michigan, and New York.
* Despite the reductions, opioid use was prevalent among nonsurgical claims with more than seven days of lost time. In 2013/2015, about 65 to 75 percent of these injured workers with pain medications received at least one opioid prescription in most of the study states. The proportion was higher in Arkansas (85 percent), Louisiana (80 percent), and South Carolina (80 percent).
* The average amounts of opioids received in Louisiana, New York, and Pennsylvania continued to be the highest among the 26 study states for claims with opioids. Although New York is among the states with a higher-than-typical amount, it is important to note the substantial decrease in both the frequency and amount of opioids in New York over the study period.
* The study observed a sizable percentage of claims with opioids that were receiving chronic opioids (at least 60 days of opioids supply over any 90-day period) and at higher doses (average daily dose of opioids exceeding 50 and 90 morphine equivalent milligrams).
* Among claims with opioids, simultaneous use of opioids with at least one other sedating drug was seen in one-third to one-half of injured workers across the 26 states. Muscle relaxants and opioids were dispensed together in 28-48 percent of claims with opioids. Use of both opioids and benzodiazepines at the same time was seen in 0-9 percent of claims.
This study uses data comprising over 430,000 nonsurgical workers’ compensation claims and nearly 2.3 million prescriptions associated with those claims from 26 states. We observed prescription utilization over an average two-year period after the injury for claims with injuries arising from October 1, 2009, to September 30, 2013. The data included in this study represent 36-69 percent of workers’ compensation claims in each state.
The 26 states included in this study are Arkansas, California, Connecticut, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Missouri, Nevada, New Jersey, New York, North Carolina, Pennsylvania, South Carolina, Tennessee, Texas, Virginia, and Wisconsin. These states represent over two-thirds of the workers’ compensation benefits paid in the United States.
To download a copy of this study, visit WCRI’s website at https://www.wcrinet.org/reports/interstate-variations-in-use-of-opioids-4th-edition. The study was authored by Vennela Thumula, Dongchun Wang, and Te-Chun Liu.
Still a long way to go, though.


- Curl of the Burl - Tuesday, Jun 27, 17 @ 9:47 am:
Good - and if AG Sessions really puts the screws to states who have med-mar programs then I hope AG Madigan and other AGs band together to sue the feds.
- Liberty - Tuesday, Jun 27, 17 @ 11:25 am:
http://khn.org/news/patients-with-mental-disorders-get-half-of-all-opioid-prescriptions/